★ Beat print – get early access to the news by signing up to the Shooting Times newsletter here ★
Hypothyroidism in dogs. What owners need to know

Q: My lab bitch is only seven years old but is acting much older. She is a little heavy, there’s hair loss and thick, scabby skin below her neck and tummy and her coat is a bit thin on her sides. Is she just getting old before her time?
A: It would seem most likely that your dog has an underactive thyroid, referred to as hypothyroidism. In very large breeds, the condition occurs between two and three years old, but in labradors and retrievers, it is between six and 10 years before it starts to develop and cause problems.(Read more on gundog health here.)
Rat tail
Q: Help! My retriever’s tail looks like it belongs to a rat, because the hair has all but fallen out.
A: Once seen, never forgotten, ‘rat tail’ is the consequence of an underactive thyroid gland (hypothyroidism). Various studies have shown that hypothyroidism will affect the skin in 60-80% of cases. Hair loss, which is usually non-itchy, bilaterally symmetrical and affects the flanks, is most common, but the tail can also become bald, especially along the top surface. Scaling and loss of quality of the coat, so that it becomes dry but greasy, are also seen. Any dog that suffers from recurrent skin infections (pyoderma) should also have its thyroid function checked. The good news is that your vet should be able to diagnose the problem on a single blood sample and, with the correct treatment, the tail can recover to its once-luxurious state in a couple of months. Because hypothyroidism tends to occur in older dogs, owners often attribute the common signs (lethargy, cold intolerance, weight gain, to old age.
Underactive thyroid – known as hypothyroidism
The clinical signs are:
- Lethargy
- Weight gain
- Bilaterally symmetrical alopecia
- Skin changes
- Itchy skin
What is the thyroid gland?
- The thyroid is situated in the neck and is part of the endocrine system.
- It uses Iodine to produce two main hormones; Triiodothyronine (T3) and Thyroxine (T4). A part of the brain called the hypothalamus produces Thyroid Releasing Hormone (TRH), which influences the pituitary gland to release varying amounts of Thyroid Stimulating Hormone (TSH), which in turn causes the thyroid to secrete T3 and T4.
- The latter are involved in many metabolic processes, including the regulation of the circulatory, respiratory, nervous and reproductive systems and they affect weight and body temperature.
What goes wrong?
The most common cause of an underactive thyroid is an auto-immune condition called lymphocytic thyroiditis.
Abnormal cells invade the gland, resulting in progressive, irreversible destruction and fibrosis of the follicles. In these patients, blood samples sent to the lab can show antibodies to thyroglobulin. Other dogs are affected by Idiopathic Atrophy, which appears to be a degenerative disorder in which normal thyroid tissue is replaced by fat cells. Rarely, tumours of the thyroid can occur.
The bottom line is, whatever the cause, destruction of normal thyroid tissue results in negative feedback to the hypothalamus and pituitary so that increased TRH and TSH squeeze every last bit of T3 and T4 out of the remaining gland. When more than 75 per cent of the thyroid is lost, however, T3 and T4 levels drop and this affects nearly every body tissue.
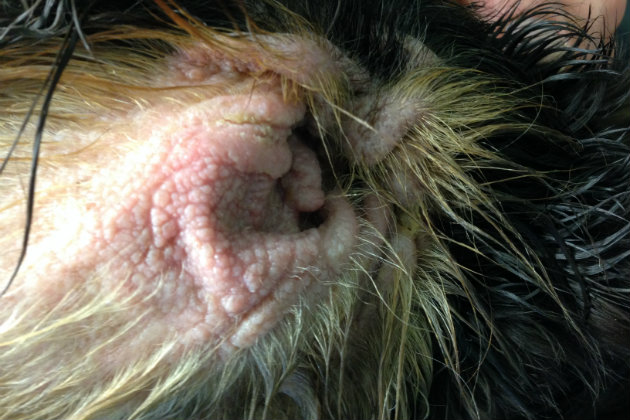
Dogs with hypothyroidism will experience moist and inflamed ears
What happens next?
- Well, lots of bad stuff really. Owners will notice lethargy, mental depression, weight gain and coat changes.
- There will be hair loss around the axillae, neck, tummy and sides, which will eventually become bilaterally symmetrical.
- The hair becomes dull, thin and brittle and a reduced ability to combat infection often results in smelly, scaly, itchy skin, which can be mistaken for allergic skin disease.
- Clipped hair is usually slow to grow back in.
- The skin eventually becomes thickened, hyper-pigmented and puffy.
- The ears are often moist and inflamed.
- Some dogs exhibit a “tragic” expression and have a pot-bellied appearance.
- The heart rate is slowed and damage to nervous tissue can result in facial nerve paralysis (think Bell’s palsy), muscle wastage and laryngeal paralysis (think noise when breathing).
- Reproduction is impaired and fatty deposits in the eye, dry eye and corneal ulceration can occur.
How is hypothyroidism diagnosed?
Look at some old photographs of your dog and you will see the difference! Otherwise, diagnosis is based on patients exhibiting a number of clinical signs along with blood changes. These include anaemia, abnormal platelet counts and increases in cholesterol, fats and liver enzymes.
Low serum T4 (below 15nmol/l) is highly suggestive of hypothyroidism but studies have shown that 60 per cent of dogs with severe illness that is not of thyroid origin will have low T4, so caution must be applied.
Serum TSH can be measured and a high result (along with a low T4) suggests hypothyroidism but 25 per cent of hypothyroid dogs will have normal TSH levels! (Now is the moment that should feel sympathy towards your poor vet!)
Is there any treatment?
Yes! And it is simple! Daily tablets or a liquid will replace lost hormone and blood levels can be monitored to ensure proper dosing, as excessive (or inappropriate) treatment can result in toxicosis.
Related Articles
Get the latest news delivered direct to your door
Subscribe to Shooting Times & Country
Discover the ultimate companion for fieldsports enthusiasts with Shooting Times & Country Magazine, the UK’s leading weekly publication that has been at the forefront of shooting culture since 1882. Subscribers gain access to expert tips, comprehensive gear reviews, seasonal advice and a vibrant community of like-minded shooters.
Save on shop price when you subscribe with weekly issues featuring in-depth articles on gundog training, exclusive member offers and access to the digital back issue library. A Shooting Times & Country subscription is more than a magazine, don’t just read about the countryside; immerse yourself in its most authoritative and engaging publication.







